When it comes to your smile, most people focus on the brightness and straightness of their teeth, but having healthy gums vs. unhealthy gums matters just as much, if not more. Your gums are the foundation of your entire smile, and understanding what healthy gum tissue looks like, versus gums that are signaling a problem, is one of the most important things you can do for your long-term oral health and overall health.
What Do Healthy Gums Look Like?
Many people don’t realize there’s a problem with their gums until symptoms become noticeable, but by then, some damage may already be done. Knowing what normal, healthy gums look and feel like gives you a baseline to spot when something has changed.
Color and Texture of Healthy Gums
Healthy gums are typically a consistent coral pink color, though the exact shade can vary slightly depending on a person’s natural skin tone and pigmentation. What’s most important is consistency. Your gums should look uniform in color without patches of redness, white areas, or dark spots. In terms of texture, healthy gums have a firm, stippled surface that resembles the skin of an orange. This texture is a sign of strong, dense gum tissue that is properly attached to your teeth and underlying bone. Puffy, smooth, or shiny-looking gums, on the other hand, are often a sign of inflammation and a warning that something may be off.
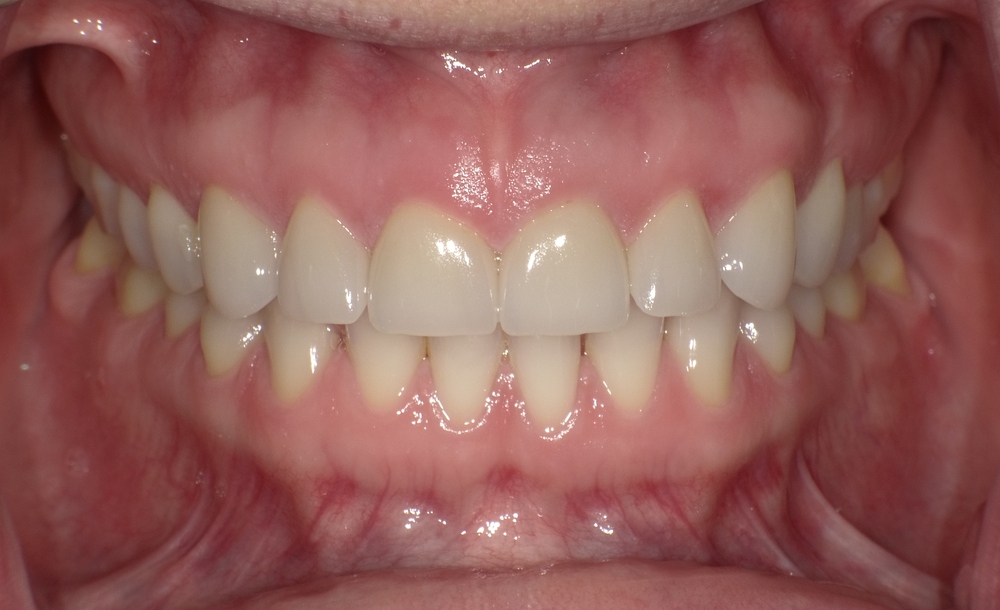
How Healthy Gums Should Feel
Beyond appearance, healthy gums should feel firm and resilient when you press on them lightly. They should not bleed when you brush or floss, and you should not experience tenderness or pain during routine oral hygiene. Healthy gums also do not feel swollen or spongy. If your gums ache, feel sensitive to temperature, or bleed with the lightest touch, these are important signs that your gums need attention. Healthy gums hold tightly to your teeth without creating pockets where bacteria can accumulate and cause damage over time.
What a Healthy Gum Line Looks Like Around Teeth
The gum line, the edge where your gums meet your teeth, should follow a smooth, scalloped curve that fits snugly around each tooth. Healthy gums sit at an appropriate height on the tooth, neither too high nor too low. There should be no visible gaps or dark spaces between the gums and the base of your teeth. The gum line should also be symmetrical and even from tooth to tooth. When the gum line starts to pull back from the tooth surface, or when you notice uneven edges, these can be early signs of gum disease or receding gums that deserve prompt evaluation by a dental professional.
What Do Unhealthy Gums Look Like? Common Warning Signs
Recognizing the signs of unhealthy gums early is critical to preventing permanent damage. Unlike tooth decay, which you might feel as pain or sensitivity, gum disease often progresses silently in its early stages. Here are the most important warning signs to watch for.
Red, Swollen, or Puffy Gums
One of the earliest and most common signs of unhealthy gums is a change in color and texture. Red gums, especially when they appear bright red or deep crimson rather than a healthy pink, indicate inflammation, which is the body’s response to bacterial infection. Swollen or puffy gums are another telltale warning sign. When bacteria build up along the gum line, the body triggers an inflammatory response that causes the tissue to swell. This puffiness may make your gums look enlarged or feel tender to the touch. Red, swollen gums that bleed easily are a classic sign of gingivitis, the earliest and most reversible stage of gum disease. Don’t ignore these changes. They are your body telling you it needs help.
Bleeding When Brushing or Flossing
Many people dismiss bleeding gums as a result of brushing too hard, but consistent bleeding when brushing or flossing is not normal and should never be ignored. Healthy gums do not bleed during routine care. When gums bleed regularly, it typically means they are inflamed and infected with bacteria that are causing tissue breakdown. Bleeding gums are one of the most recognizable signs of gingivitis and should be treated as an early warning sign of gum disease. If you notice blood on your toothbrush or in the sink when you spit, schedule a visit with your dentist or periodontist to evaluate the health of your teeth and gums as soon as possible.
Receding Gums and Exposed Tooth Roots
Receding gums occur when the gum tissue pulls away from the teeth, exposing more of the tooth’s surface and sometimes the root itself. This is a significant sign of unhealthy gums and should be addressed quickly. Receding gums can be caused by aggressive brushing, gum disease, or genetics. Once gum tissue recedes, it does not grow back on its own, which is why early treatment is so important. Exposed roots are not only aesthetically concerning. They also increase tooth sensitivity and vulnerability to decay. If you notice your teeth looking longer than they used to, or if you can feel a ridge where your tooth meets exposed root tissue, talk to your dentist right away.
Persistent Bad Breath or Bad Taste in the Mouth
Occasional bad breath after meals or in the morning is perfectly normal. But persistent bad breath, also known as halitosis, that doesn’t go away with brushing and rinsing, can be a sign of gum disease. Bacteria that collect in deep pockets between the gums and teeth produce sulfur compounds that cause a chronic, unpleasant odor or taste. If you consistently experience bad breath even with good oral hygiene, or if you notice a foul taste that lingers, this is one of the signs of unhealthy gums that warrants professional evaluation. It may indicate that bacteria are thriving in areas that your toothbrush and floss cannot adequately reach.
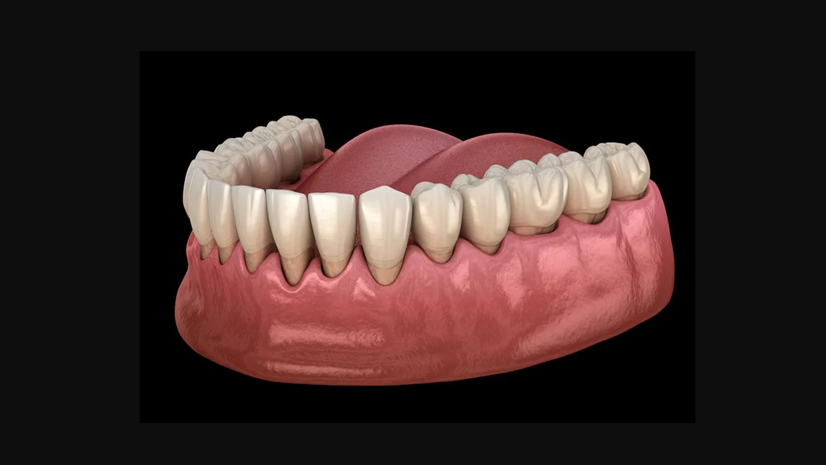
Stages of Gum Disease: From Gingivitis to Periodontitis
Understanding the stages of gum disease can help you appreciate the urgency of early treatment and the consequences of leaving gum problems unaddressed. Gum disease is not a single condition; it exists on a spectrum that ranges from mild and reversible to severe and permanent.
What Is Gingivitis and Is It Reversible?
Gingivitis is the earliest stage of gum disease and is defined by inflammation of the gum tissue caused by plaque and bacterial buildup along the gum line. The good news is that gingivitis is fully reversible with prompt and proper treatment. At this stage, there is no permanent damage to the bone or connective tissue that supports your teeth. A sign of gingivitis includes gums that are red, swollen, and bleed easily. Many patients with gingivitis experience no pain, which is why it can go unnoticed. A professional dental cleaning combined with improved at-home oral hygiene, including proper brushing and flossing, is usually enough to resolve gingivitis and restore gum health. Regular checkups are critical for catching gum disease at this manageable stage.
What Happens When Gingivitis Progresses to Periodontitis
When gingivitis is left untreated, it can advance to periodontitis – a more serious form of gum disease that involves irreversible damage to the structures that support your teeth. In periodontitis, the inner layer of the gum and bone pull away from the teeth and form pockets. These spaces between teeth and gums become infected, and as the immune system fights the bacteria, the toxins produced begin to break down the bone and connective tissue that hold teeth in place. Unlike gingivitis, the bone loss associated with periodontitis cannot be fully reversed, though treatment can stop its progression. Periodontal disease is one of the leading causes of tooth loss in adults and requires professional intervention to manage effectively.
Signs Your Gum Disease Has Become Advanced
Advanced periodontitis presents with increasingly serious symptoms that go well beyond red or bleeding gums. At this stage, patients may notice loose or shifting teeth, significant changes in how their bite feels, or teeth that appear to have moved position. Deep pockets between the teeth and gums are a hallmark of advanced disease, and patients often experience persistent pain, significant bad breath, and visible pus between the teeth and gums. In severe cases, tooth loss becomes unavoidable without aggressive treatment. Advanced gum disease also correlates strongly with systemic health complications, making it even more urgent to address. If you recognize any of these advanced signs of gum disease, seek care from a dentist or periodontist without delay.
What Causes Unhealthy Gums?
Gum disease rarely develops overnight. It is typically the result of a combination of factors, some within your control, and others that require extra vigilance due to predisposition.
Poor Oral Hygiene and Plaque Buildup
The most common and preventable cause of unhealthy gums is inadequate oral hygiene. When plaque is not consistently removed through brushing and flossing, it hardens into tartar (also called calculus) along the gum line. Tartar cannot be removed with a toothbrush and provides a rough surface where more bacteria can adhere. Over time, these bacteria produce toxins that irritate the gum tissue, triggering the inflammation that leads to gingivitis and, eventually, periodontal disease. Brushing twice daily, flossing at least once a day, and attending regular professional cleanings are the cornerstones of healthy gum maintenance.
Smoking and Tobacco Use
Tobacco use in any form is one of the most significant risk factors for gum disease. Smoking reduces blood flow to the gums, which impairs the tissue’s ability to heal and fight infection. It also masks some of the classic warning signs of gum disease. For example, smokers are less likely to experience bleeding gums, which can give a false sense of security while the disease progresses silently. Smokeless tobacco products cause direct tissue damage to the gums and the lining of the mouth. Research consistently shows that smokers are significantly more likely to develop severe and treatment-resistant gum disease than non-smokers. Quitting tobacco use is one of the most impactful steps a person can take for their gum health.
Hormonal Changes, Medications, and Health Conditions
Hormonal changes, particularly during pregnancy, puberty, and menopause, can make gum tissue more sensitive to inflammation. “Pregnancy gingivitis” is a well-documented phenomenon in which elevated hormone levels increase the gum response to plaque. Certain medications, including some blood pressure drugs, anticonvulsants, and immunosuppressants, can cause gum overgrowth or dry mouth, both of which increase disease risk. Systemic conditions like diabetes also have a well-established bidirectional relationship with gum disease, meaning each condition can worsen the other. If you take medications or have a chronic health condition, talk to your dentist about what that means for your gum health management.
Genetics and Other Risk Factors
Even people with excellent oral hygiene habits can be predisposed to gum disease due to genetics. Research suggests that up to 30% of people have a genetic susceptibility that makes them significantly more likely to develop periodontal disease regardless of how well they care for their teeth. Stress, a diet high in sugar and processed foods, vitamin deficiencies, and certain immune disorders can also increase gum disease risk. Understanding your personal risk profile allows you and your dental provider to develop a more targeted prevention and monitoring plan that fits your unique needs.
Why Gum Health Affects Your Whole Body
The relationship between gum health and overall health is one of the most important and compelling findings in modern dentistry. The mouth is not separate from the rest of the body. (It is a gateway, and what happens in your gums can have profound effects on your systemic health.
The Link Between Gum Disease and Heart Disease
Multiple large-scale studies have found a significant association between periodontal disease and cardiovascular disease, including heart attack and stroke. Researchers believe that the bacteria associated with gum disease can enter the bloodstream through inflamed gum tissue and travel to the heart and arteries, contributing to inflammation in blood vessels and the buildup of arterial plaques. While the exact nature of the cause-and-effect relationship is still being studied, the correlation is strong enough that cardiologists and dentists increasingly recommend coordinated care for patients with both conditions. Maintaining healthy gums may be one meaningful way to reduce cardiovascular risk.
Gum Disease and Diabetes
The relationship between gum disease and diabetes is bidirectional and well-documented. People with diabetes are more susceptible to gum infections because high blood sugar impairs immune response and slows healing. Conversely, chronic gum infection makes it harder to control blood sugar levels, potentially worsening diabetes management. Studies have shown that treating gum disease can lead to modest but meaningful improvements in blood glucose control. If you have diabetes, excellent gum care is not optional. It is an integral part of managing your overall health and preventing complications.
Other Systemic Health Conditions Connected to Unhealthy Gums
The connections between oral health and systemic health extend beyond the heart and diabetes. Research has linked periodontal disease to respiratory infections (since bacteria in the mouth can be inhaled into the lungs), adverse pregnancy outcomes, including preterm birth and low birth weight, rheumatoid arthritis, and kidney disease. Some studies are also exploring potential links to cognitive decline and certain cancers, though research in these areas is ongoing.
How to Get Healthy Gums Back
The encouraging news is that in many cases, especially when gum disease is caught early, healthy gums can be restored with the right combination of professional treatment and consistent at-home care.
Professional Treatments for Gum Disease
For early-stage gum disease (gingivitis), a professional dental cleaning combined with improved home care is often sufficient to reverse the condition. For more advanced cases, your dentist or periodontist may recommend scaling and root planing, a deep cleaning procedure that removes plaque and tartar from beneath the gum line and smooths the root surface to help the gums reattach. In cases of severe periodontal disease, surgical interventions such as flap surgery, bone grafting, or gum grafting may be necessary to restore lost tissue and bone. Laser therapy is also increasingly used as a minimally invasive option for treating infected gum pockets. Your provider will tailor a treatment plan to the specific stage and severity of your condition.
At-Home Habits That Improve Gum Health
Professional treatment creates the foundation, but consistent daily habits are what sustain healthy gums over the long term. Brush your teeth at least twice daily with a soft-bristle toothbrush, using gentle circular motions along the gum line. Floss at least once a day to remove plaque and food debris from between teeth where your toothbrush cannot reach. An antimicrobial mouthwash can provide additional protection by reducing bacterial levels in the mouth. Eat a balanced diet rich in vitamins C and D, which support gum tissue health and immune function. Drink plenty of water, quit tobacco if you use it, and keep up with regular dental appointments, typically every six months, or more frequently if you have a history of gum disease.
Concerned About Your Gum Health? Visit Ashley Harrison, DDS
Understanding healthy vs unhealthy gums is the first step toward protecting your smile. Whether you’ve noticed the early signs of gum problems or simply want to stay ahead of any issues, Dr. Ashley Harrison is here to help. Our practice provides comprehensive gum evaluations, personalized treatment plans, and supportive care to help you achieve and maintain a healthy, confident smile. Don’t wait for symptoms to worsen. Schedule your appointment with Ashley Harrison, DDS, today and take the first step toward gums that truly support your health and your smile.
Frequently Asked Questions
What is the difference between healthy and unhealthy gums?
Healthy gums are firm, coral pink in color, and fit snugly around each tooth without bleeding, swelling, or discomfort. They have a slightly textured, stippled surface and sit at a consistent gum line. Unhealthy gums, by contrast, may appear red or dark, feel swollen or spongy, bleed during brushing or flossing, and pull away from the teeth. As gum disease progresses, unhealthy gums can lead to deep pockets between the teeth and gums, receding gum tissue, exposed roots, and eventually tooth loss. The key difference comes down to the presence of bacterial infection and inflammation. Healthy gums are infection-free and well-attached to supporting bone and tissue, while unhealthy gums are in various stages of breakdown caused by bacterial buildup. Regular dental checkups are the most reliable way to evaluate gum health.
Can unhealthy gums become healthy again?
Yes, in many cases, unhealthy gums can become healthy again, particularly when gum disease is caught in its early stages. Gingivitis, the earliest form of gum disease, is fully reversible with professional cleaning and improved oral hygiene at home. Even in more advanced cases of periodontitis, while the bone loss cannot be fully reversed, treatment can stop the disease from progressing and restore gum stability. Options like scaling and root planing, antibiotic therapy, and in some cases, surgical procedures can significantly improve gum health. The key is acting promptly. The longer gum disease is left untreated, the more difficult and costly the recovery becomes. With the right professional treatment plan and consistent at-home care, many patients experience dramatic improvements in their gum health and overall oral well-being.
What color should healthy gums be?
Healthy gums are typically a coral pink color, though the exact shade can vary from person to person based on natural skin tone and melanin levels. In individuals with darker complexions, healthy gums may have more natural pigmentation and appear darker or brownish. This is completely normal. What matters most is consistency in color across the gum tissue. Gums that are bright red, deep red, purple, or that have patchy white areas are indicating inflammation, infection, or another problem that should be evaluated by a dental professional. Pale gums can sometimes indicate anemia or poor circulation. If you are ever uncertain whether the color of your gums is normal, the best step is to have your dentist take a look. They can assess whether the color is within a healthy range for your individual baseline.
Why do my gums bleed when I brush my teeth?
Bleeding gums during brushing are one of the most common signs of gingivitis and should not be dismissed as simply brushing too hard. While aggressive brushing can cause occasional bleeding, consistent or regular bleeding is almost always a sign of gum inflammation caused by plaque and bacteria along the gum line. When gum tissue is infected and inflamed, the blood vessels within it become engorged and fragile, making them prone to bleeding with minimal contact. The good news is that if the bleeding is due to gingivitis, improving your brushing technique, flossing daily, and getting a professional cleaning can resolve it relatively quickly. However, if bleeding gums persist even with improved care, it may indicate a more advanced stage of gum disease or another underlying issue that requires professional evaluation and treatment.
How do I know if I have gum disease?
The signs of gum disease can range from subtle in early stages to quite obvious in more advanced cases. Common indicators include red, swollen, or tender gums, bleeding when you brush or floss, persistent bad breath that does not resolve with brushing, gums that are pulling away from your teeth, changes in how your teeth fit together when you bite, and loose or shifting teeth. In the very early stage, many people have no pain at all, which is why regular dental checkups are so important. A dentist can measure the depth of the pockets around your teeth using a small probe, take X-rays to evaluate bone levels, and identify disease that is not yet producing noticeable symptoms. If you have any of the warning signs described above, schedule an appointment as soon as possible to get a proper diagnosis and begin treatment.


